Home » Diseases » Emergencies / First Aid for Dogs & Cats – General Information » Emergencies / First Aid A-Z » Bruising (hematoma)
Bruising (hematoma)
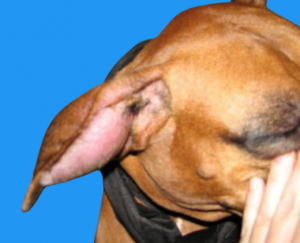 Bruising (hematoma) on the ear (aural hematoma)
Bruising (hematoma) on the ear (aural hematoma)
You might also be interested in:
Definition
Bruising (hematoma)
A hematoma is a local collection of blood in the tissue as a result of a vascular injury, usually due to traumaA trauma refers to a physical injury or damage caused by external force. Traumas can range from simple cuts to severe multiple injuries. or coagulationCoagulation is the process of blood coagulation, in which liquid blood is transformed into a solid clot. This process is crucial for stopping Bleeding and promoting wound healing. disorders. Typical symptoms include swelling, pain, and a blue-red-violet discoloration of the skin. Large hematomas can cause pressure damage or indicate internal bleeding.
A bruising (hematoma), medically referred to as a hematoma, is caused by the accumulation of blood outside the blood vessels in the tissue. This process involves the ruptureA rupture is a tear or break in an organ or tissue. It can be caused by trauma, illness, or overextension, and often requires medical intervention. of blood vessels, causing blood to leak into the surrounding tissue and accumulate there. Hematomas can occur both superficially under the skin (subcutaneousSubcutaneous means “under the skin.” In medicine, it refers to the administration of drugs or the placement of implants directly under the skin.) and in deeper tissue layers such as muscles, organs, or body cavities. In dogs and cats, we distinguish between different types of hematomas, which differ in their location and mode of origin. SubcutaneousSubcutaneous means “under the skin.” In medicine, it refers to the administration of drugs or the placement of implants directly under the skin. hematomas, which form directly under the skin and become visible as bluish-violet discolorations, and aural hematomas, which occur specifically on the auricle, are particularly common. The formation of a hematoma is part of the body’s own reaction to a tissue injury and represents the first step in the healing process. The leaked blood initially clots and is then resorbed by the body over time, with characteristic color changes from dark red to blue-violet to yellowish-green.
Causes
Bruising in pets occurs through various mechanisms, all of which lead to damage to blood vessels. The most common cause is blunt traumas such as bumps, falls, or collisions, where the skin remains intact, but underlying vessels ruptureA rupture is a tear or break in an organ or tissue. It can be caused by trauma, illness, or overextension, and often requires medical intervention.. In dogs, bruising (hematoma) often occurs after fights with other dogs, traffic accidents, or bumping into furniture. Cats often sustain bruising from falls from heights or territorial fights. A special form is the aural hematoma, which is caused by vigorous head shaking due to ear infections or foreign bodies in the ear canal, where blood vessels ruptureA rupture is a tear or break in an organ or tissue. It can be caused by trauma, illness, or overextension, and often requires medical intervention. between the ear cartilage and skin. Surgical procedures can also lead to hematomas, especially if blood coagulationBlood coagulation is a process that helps stop Bleeding when a blood vessel is damaged. Platelets and certain proteins in the plasma form a blood clot that seals the wound. during the operation was inadequate or postoperativePostoperative refers to the time after a surgical operation. This phase includes recovery and the management of possible complications after the procedure. activity is increased. In older animals or animals with certain underlying diseases, hematomas can also occur spontaneously or after minimal traumas. This can be due to coagulationCoagulation is the process of blood coagulation, in which liquid blood is transformed into a solid clot. This process is crucial for stopping Bleeding and promoting wound healing. disorders such as von Willebrand disease, thrombocytopeniaThrombocytopenia is a condition in which the number of platelets in the blood is lower than normal, increasing the risk of mild to severe Bleeding., liver diseases, or the use of anticoagulantsAnticoagulants are medications that slow down or inhibit blood coagulation. They are used to prevent the formation of blood clots and are used in dogs and cats with certain heart conditions or coagulation disorders.. TumorA tumor is an abnormal growth of tissue that can be benign or malignant. Tumors can develop in any part of the body and affect various functions. diseases, especially hemangiosarcomas, can also lead to spontaneous bleeding and hematomas.
Symptoms
Bruising (hematoma) in dogs and cats
Typical Symptoms:
- Local swelling, discoloration, pain on palpationPalpation is an examination method in which the condition of body tissues is assessed by feeling them with the hands. It is used to identify swelling, pain, or other abnormalities./pain on palpation
- After traumaA trauma refers to a physical injury or damage caused by external force. Traumas can range from simple cuts to severe multiple injuries./bumping, possibly lameness
- Aural hematoma: swollen, warm ear, head shaking
Alarm signs:
- Rapidly growing hematoma, very painful
- Hematomas without recognizable traumaA trauma refers to a physical injury or damage caused by external force. Traumas can range from simple cuts to severe multiple injuries. or in multipleMultiple means manifold or repeated and is used to describe conditions or events that occur in multiple instances or at different locations. In veterinary medicine, this may indicate multiple lesions, tumors, or other pathological changes. locations
- Pale mucous membranes, weakness (internal blood loss possible)
- Hematoma on the neck/thorax / chest/abdomen after an accident → internal traumaA trauma refers to a physical injury or damage caused by external force. Traumas can range from simple cuts to severe multiple injuries. possible
Escalation/course:
- Increase in size in minutes–hours → active bleeding/vascular damage
- Aural hematoma becomes firmer + deformation in days → therapyTherapy refers to the treatment of diseases or disorders with the aim of alleviating symptoms, promoting healing, or improving quality of life. Therapies can be medicinal, surgical, or through other medical interventions. makes sense in a timely manner
- Later: infectionAn infection is the colonization and multiplication of pathogens such as bacteria, viruses, fungi, or parasites in an organism, which often, but not always, leads to a disease./abscess possible if punctured/manipulated
The appearance of a bruising (hematoma) varies depending on the location, size, and age of the injury. Superficial subcutaneousSubcutaneous means "under the skin." In medicine, it refers to the administration of drugs or the placement of implants directly under the skin. hematomas manifest as visible, initially reddish-bluish, later greenish-yellow discoloration of the skin. They are often associated with swelling, which can vary in intensity depending on the extent of the bleeding. On palpationPalpation is an examination method in which the condition of body tissues is assessed by feeling them with the hands. It is used to identify swelling, pain, or other abnormalities., fresh hematomas feel firm and elastic and are typically painful. Animals often show lameness or protective posture / guarding posture if limbs are affected. Aural hematomas result in a characteristic fluctuating, doughy swelling of the auricle, which can lead to deformation. Affected animals often shake their heads or scratch their ears more frequently. Deeper hematomas in muscles or organs may not be visible externally and manifest as non-specific symptoms such as unwillingness to move, pain on palpationPalpation is an examination method in which the condition of body tissues is assessed by feeling them with the hands. It is used to identify swelling, pain, or other abnormalities., or impaired function of the affected organ. Large or massive bruising (hematoma) can lead to relevant blood loss, which manifests as pale mucous membranes, increased heart rate, and weakness. In the course of healing, the appearance of the hematoma changes: the swelling decreases, the color changes from dark red to blue-violet to green-yellow, and the pain subsides.
Special considerations for cats
After a fall/road traffic accident, internal injuries may be present despite few external signs. If there is an increased breathing rate (tachypneaTachypnea or tachypoe refers to an increased respiratory rate that is above the normal range for the respective living being. It may be a sign of shortness of breath or other respiratory diseases.) or Low body temperature (hypothermia), go to the vet immediately.
First Aid
- No treatment is often necessary for minor bruising (hematoma).
- Immediate cooling (ice pack) for 10 to 20 minutes, possibly several times within 24 hours, and rest, at least for the next few hours, prevents or slows down further blood leakage from the injured blood vessel.
- If a large bruising (hematoma) is forming, a pressure bandage can be applied for a short time (maximum 20 minutes) while cooling.
- After that, however, you should remove the bandage, as there is often a lack of experience in how strong the applied pressure should be. The blood circulation and thus the supply of nutrients to the tissue must not be prevented!
- It is better to leave head bandages for an aural hematoma to your veterinarian.
- Do not open an aural hematoma yourself.
When should you see a vet sooner?
Urgency increases from Green to → Yellow/Orange in cases of rapid growth, severe pain, pallor/weakness, or suspected clotting disorder/trauma.
Diagnosis
The diagnosisA diagnosis is the identification of a disease or condition by its symptoms and/or results from diagnostic tests. It is the first step in the management and treatment of patients. of a bruising (hematoma) is primarily made through clinical examination. The veterinarian pays attention to typical signs such as swelling, discoloration of the skin, and pain on palpationPalpation is an examination method in which the condition of body tissues is assessed by feeling them with the hands. It is used to identify swelling, pain, or other abnormalities.. The medical historyThe medical history is the systematic collection of a patient's medical history through questioning. It includes information about previous illnesses, treatments, allergies, and lifestyle habits. plays an important role in identifying possible causes such as traumas or underlying diseases. The diagnosisA diagnosis is the identification of a disease or condition by its symptoms and/or results from diagnostic tests. It is the first step in the management and treatment of patients. is usually straightforward for superficial hematomas. Imaging techniques may be necessary for deeper hematomas or to clarify the extent. UltrasoundUltrasound refers to sound waves that are above the hearing threshold of the human ear. In medicine, ultrasound is used for diagnostic imaging procedures to visualize internal organs, tissues, and blood flow. examinations allow the visualization of fluid accumulations in the tissue and help to assess the size of the hematoma and possible involvement of deeper structures. X-rays may be indicated if bone fractures or organ injuries are suspected. In more complex cases, computed tomography (CT) or magnetic resonance imaging (MRI)Magnetic resonance imaging is an imaging technique that uses strong magnetic fields and radio waves to create detailed images of the inside of the body. It is used in veterinary medicine to diagnose diseases of the brain, spine, and other organs. are used. In the case of recurrentRecurrent refers to a disease that repeatedly returns or worsens after a temporary remission or improvement. or spontaneously occurring hematomas, further diagnostics should be carried out to identify possible underlying diseases. These include blood tests to assess blood coagulationBlood coagulation is a process that helps stop Bleeding when a blood vessel is damaged. Platelets and certain proteins in the plasma form a blood clot that seals the wound. function (plateletsPlatelets, also called thrombocytes, are cells in the blood that play a crucial role in blood coagulation. They help stop Bleeding by forming clots that seal injuries in blood vessels. count, blood coagulationBlood coagulation is a process that helps stop Bleeding when a blood vessel is damaged. Platelets and certain proteins in the plasma form a blood clot that seals the wound. times), liver diagnostics, and, if necessary, specific tests for coagulationCoagulation is the process of blood coagulation, in which liquid blood is transformed into a solid clot. This process is crucial for stopping Bleeding and promoting wound healing. disorders such as the von Willebrand factorThe von Willebrand factor is a protein in the blood that plays an essential role in blood coagulation. It helps platelets bind to the site of an injury and contributes to the formation of a blood clot.. A fine-needle aspirationFine-needle aspiration is a minimally invasive diagnostic technique that uses a thin needle to extract cells or fluid from a tumor, lesion, or organ. This sample is then examined microscopically to make a diagnosis. or biopsyA biopsy is a medical procedure in which a small amount of tissue is removed from the body to be examined under a microscope for signs of disease. Biopsies can help diagnose cancer and other conditions. of the hematoma can help to differentiate it from other swelling such as tumors or abscesses in unclear cases.
Further veterinary measures
The treatment of bruising (hematoma) depends on size, location, and severity. Conservative therapyTherapy refers to the treatment of diseases or disorders with the aim of alleviating symptoms, promoting healing, or improving quality of life. Therapies can be medicinal, surgical, or through other medical interventions. is often sufficient for smaller, superficial hematomas. In the acuteAcute refers to a condition that occurs suddenly and is usually of short duration. In a medical context, it describes symptoms or illnesses that can quickly become serious and require immediate attention. phase (first 24–48 hours), cold therapyTherapy refers to the treatment of diseases or disorders with the aim of alleviating symptoms, promoting healing, or improving quality of life. Therapies can be medicinal, surgical, or through other medical interventions. is the priority: Applying cold compresses for 15–20 minutes several times a day promotes vasoconstriction and minimizes further blood leakage. After 48 hours, heat applications can be used to accelerate the resorption of the hematoma. Non-steroidalNon-steroidal refers to medications or substances that are not steroids and often have anti-inflammatory, analgesic, or antipyretic effects. They are used in dogs and cats to treat Pain and Inflammatory conditions. anti-inflammatory drugsAnti-inflammatory drugs are medications that reduce inflammation. They can be divided into nonsteroidal anti-inflammatory drugs (NSAIDs) and corticosteroids and are used in dogs and cats to reduce Inflammatory conditions and Pain. such as carprofen or meloxicam are used for pain relief, whereby kidney function should be monitored. For larger or problematic hematomas, puncture and drainageDrainage refers to the removal of fluid from body cavities, Wounds, or inflamed areas, often using a tube or other device. It is used to prevent infection and promote healing. may be necessary to remove accumulated blood and reduce pressure on the surrounding tissue. Aural hematomas usually require surgical intervention because they are rarely absorbed spontaneously. The accumulated blood is removed and re-accumulation is prevented by sutures or drainageDrainage refers to the removal of fluid from body cavities, Wounds, or inflamed areas, often using a tube or other device. It is used to prevent infection and promote healing.. At the same time, the underlying cause (e.g. ear infectionAn infection is the colonization and multiplication of pathogens such as bacteria, viruses, fungi, or parasites in an organism, which often, but not always, leads to a disease.) should be treated. In the case of hematomas due to coagulationCoagulation is the process of blood coagulation, in which liquid blood is transformed into a solid clot. This process is crucial for stopping Bleeding and promoting wound healing. disorders, the underlying disease must be treated, for example by vitaminVitamins are organic compounds that are necessary in small amounts for the normal growth, development, and physiological function of the body. Vitamins must mostly be obtained through food, as the body cannot produce them or not in sufficient quantities. K substitution in the case of poisoning by anticoagulantsAnticoagulants are medications that slow down or inhibit blood coagulation. They are used to prevent the formation of blood clots and are used in dogs and cats with certain heart conditions or coagulation disorders. or specific treatments for thrombocytopeniaThrombocytopenia is a condition in which the number of platelets in the blood is lower than normal, increasing the risk of mild to severe Bleeding.. In severe cases with significant blood loss, blood transfusions may be necessary. Immobilization of the affected body part is an important part of the therapyTherapy refers to the treatment of diseases or disorders with the aim of alleviating symptoms, promoting healing, or improving quality of life. Therapies can be medicinal, surgical, or through other medical interventions. to prevent further bleeding.
Prognosis and aftercare
The prognosis for bruising (hematoma) is favorable in most cases. Smaller, superficial hematomas usually heal completely within 2–3 weeks without leaving any permanent damage. However, the healing time can vary depending on the size, location, and underlying diseases of the animal. The healing process may take longer for larger hematomas or those in sensitive areas. Aural hematomas tend to recur without adequate surgical care or can lead to permanent deformation of the auricle. Follow-up care includes regular checks of the healing process, paying attention to signs of infectionAn infection is the colonization and multiplication of pathogens such as bacteria, viruses, fungi, or parasites in an organism, which often, but not always, leads to a disease. such as increasing redness, warmth, or purulentPurulent refers to pus or the production of pus, which may indicate a bacterial infection. Purulent inflammatory conditions are often painful and may have significant swelling and redness. discharge. In the case of surgically treated hematomas, dressing changes and suture removal must be carried out according to veterinary instructions. The animal’s activity should be restricted during the healing phase to avoid renewed traumas. It is particularly important to identify and treat underlying diseases in the case of recurring or spontaneously occurring hematomas. A lick guard may be necessary to prevent the animal from licking or biting the affected area. In the case of aural hematomas, follow-up care is particularly important to avoid recurrence. This includes consistent treatment of ear infections and regular ear hygiene.
Summary
Bruising (hematoma) are common consequences of injuries in pets, which are caused by the leakage of blood into the tissue after vascular injuries. They can occur superficially under the skin or in deeper tissue layers and typically manifest as painful swelling with characteristic discoloration. The most common causes are blunt traumas, with vigorous head shaking due to ear infections specifically causing aural hematomas. The diagnosisA diagnosis is the identification of a disease or condition by its symptoms and/or results from diagnostic tests. It is the first step in the management and treatment of patients. is primarily clinical but can be supplemented by imaging techniques and laboratory tests, especially if underlying diseases are suspected. Therapeutically, conservative treatment with cooling, pain relievers, and immobilization is the priority for smaller hematomas, while larger or problematic hematomas may require drainageDrainage refers to the removal of fluid from body cavities, Wounds, or inflamed areas, often using a tube or other device. It is used to prevent infection and promote healing. or surgical intervention. The prognosisThe prognosis is the prediction of the likely course and outcome of a disease based on the general state of health, the nature of the disease, and the response to treatment. It can provide information on how a disease is expected to develop. is generally good, with the healing time depending on various factors. Careful follow-up care and treatment of underlying diseases are important to avoid complications and recurrence. Recurring or spontaneously occurring hematomas deserve special attention, as they may indicate coagulationCoagulation is the process of blood coagulation, in which liquid blood is transformed into a solid clot. This process is crucial for stopping Bleeding and promoting wound healing. disorders or other systemic diseases.
Outlook on current research
Veterinary research on hematomas is currently focused on several promising areas. Innovative treatment approaches such as the use of platelet-rich plasmaPlasma is the liquid part of blood in which blood cells are suspended. It contains water, salts, proteins, and other substances and serves as a transport medium for nutrients, hormones, and waste products. (PRP) show positive effects in initialInitial means beginning or at the start. In medicine, it can refer to the first symptoms of a disease or the first phase of a treatment process. studies on the healing speed and quality of tissue regeneration in hematomas. This form of therapyTherapy refers to the treatment of diseases or disorders with the aim of alleviating symptoms, promoting healing, or improving quality of life. Therapies can be medicinal, surgical, or through other medical interventions. uses the body’s own growth factors from concentrated plateletsPlatelets, also called thrombocytes, are cells in the blood that play a crucial role in blood coagulation. They help stop Bleeding by forming clots that seal injuries in blood vessels. to accelerate healing processes. In the field of aural hematomas, new minimally invasiveInvasive describes medical procedures or pathogens that enter the body or penetrate tissue. In medicine, invasive procedures can range from minimally invasive techniques to open surgery. surgical techniques are being developed to enable faster healing with less scar tissue formation. Laser-assisted procedures and special drainageDrainage refers to the removal of fluid from body cavities, Wounds, or inflamed areas, often using a tube or other device. It is used to prevent infection and promote healing. systems are being evaluated to reduce the recurrence rate and achieve cosmetically better results. The molecular mechanisms of hematoma resorption are being researched more intensively to develop pharmacological interventions that can accelerate natural degradation. The focus here is on inflammation-modulating substances and enzymesEnzymes are biological catalysts that accelerate specific chemical reactions in the body without being consumed. They play a crucial role in virtually all physiological processes. that specifically promote the breakdown of blood components. Advances in imaging diagnostics, in particular high-resolution ultrasoundUltrasound refers to sound waves that are above the hearing threshold of the human ear. In medicine, ultrasound is used for diagnostic imaging procedures to visualize internal organs, tissues, and blood flow. procedures and functional MRI techniques, enable a more precise assessment of hematomas and their effects on surrounding tissue. This contributes to individualized treatment strategies. Genetic studies on coagulationCoagulation is the process of blood coagulation, in which liquid blood is transformed into a solid clot. This process is crucial for stopping Bleeding and promoting wound healing. disorders in various dog and cat breeds help to identify risk populations and develop preventive measures. These research approaches promise improved diagnostic and therapeutic options for hematomas in pets in the coming years.
Frequently asked questions (FAQs)
- How long does it take for a bruising (hematoma) to heal in my pet?
Smaller hematomas usually heal within 2–3 weeks. For larger hematomas or those in unfavorable locations, healing can take 4–6 weeks or longer. - Can I treat a hematoma in my animal myself?
Small, superficial hematomas can often be treated independently by cooling in the first 24–48 hours and subsequent immobilization. A veterinarian should always be consulted for larger hematomas, severe pain, or hematomas in sensitive areas. - Why do some dogs repeatedly develop aural hematomas?
Recurring aural hematomas are often caused by chronicChronic refers to a condition or disease that is long-lasting or permanent. Chronic diseases often develop slowly and can lead to persistent or recurring health problems over time. ear infections, allergies, or foreign bodies that lead to increased head shaking. A thorough diagnosisA diagnosis is the identification of a disease or condition by its symptoms and/or results from diagnostic tests. It is the first step in the management and treatment of patients. and treatment of the underlying cause are crucial. - When is a bruising (hematoma) in my pet an emergency?
A hematoma is an emergency if it grows rapidly, is associated with severe pain, impairs breathing or other vital functionsVital functions are essential bodily functions necessary to sustain life. These include breathing, heart rate, blood pressure, body temperature, and level of consciousness., or shows signs of significant blood loss (pale mucous membranes, weakness). - Can hematomas in pets burst on their own?
Yes, large superficial hematomas can occasionally ruptureA rupture is a tear or break in an organ or tissue. It can be caused by trauma, illness, or overextension, and often requires medical intervention. spontaneously, especially if they are under tension or the animal licks/scratches them. This carries a risk of infectionAn infection is the colonization and multiplication of pathogens such as bacteria, viruses, fungi, or parasites in an organism, which often, but not always, leads to a disease. and should be treated by a veterinarian. - Are there breeds that are more prone to bruising (hematoma)?
Yes, breeds with known coagulationCoagulation is the process of blood coagulation, in which liquid blood is transformed into a solid clot. This process is crucial for stopping Bleeding and promoting wound healing. disorders such as Dobermans (von Willebrand disease) or Scottish Terriers (thrombocytopathies) are more prone to hematomas. Very active or hunting dogs also often suffer from trauma-related bruising (hematoma). - How do you distinguish a bruising (hematoma) from a tumorA tumor is an abnormal growth of tissue that can be benign or malignant. Tumors can develop in any part of the body and affect various functions. or abscess?
The distinction can be difficult because all three can appear as swelling. Hematomas typically occur after traumas and change their color during the healing process. In case of uncertainty / disorientation, a veterinary examination with ultrasoundUltrasound refers to sound waves that are above the hearing threshold of the human ear. In medicine, ultrasound is used for diagnostic imaging procedures to visualize internal organs, tissues, and blood flow. or puncture if necessary is required. - Can medications increase the risk of bruising (hematoma)?
Yes, anticoagulantsAnticoagulants are medications that slow down or inhibit blood coagulation. They are used to prevent the formation of blood clots and are used in dogs and cats with certain heart conditions or coagulation disorders. such as aspirin, warfarin, or newer anticoagulantsAnticoagulants are medications that slow down or inhibit blood coagulation. They are used to prevent the formation of blood clots and are used in dogs and cats with certain heart conditions or coagulation disorders. increase the risk of hematomas. Certain antibiotics, chemotherapeutic agents, or corticosteroidsCorticosteroids are a class of steroid hormones that occur naturally in the body and can also be produced synthetically. They have anti-inflammatory and immunosuppressive properties and are used in veterinary medicine to treat a variety of conditions. can also affect blood coagulationBlood coagulation is a process that helps stop Bleeding when a blood vessel is damaged. Platelets and certain proteins in the plasma form a blood clot that seals the wound. in rare cases. - Is a special diet useful during the healing of a hematoma?
A balanced diet supports healing. VitaminVitamins are organic compounds that are necessary in small amounts for the normal growth, development, and physiological function of the body. Vitamins must mostly be obtained through food, as the body cannot produce them or not in sufficient quantities. K-rich food can be helpful for mild coagulationCoagulation is the process of blood coagulation, in which liquid blood is transformed into a solid clot. This process is crucial for stopping Bleeding and promoting wound healing. disorders. In severe cases or specific underlying diseases, the diet should be coordinated with the veterinarian. - Can a hematoma in my animal lead to permanent damage?
In most cases, hematomas heal without permanent damage. However, large or inadequately treated hematomas can lead to scar tissue formation, calcification, or, in the case of aural hematomas, permanent deformation of the auricle.
Literature
- Ettinger, S. J., Feldman, E. C., & Côté, E. (2022). Textbook of veterinary internal medicine: Diseases of the dog and cat (9th ed., pp. 1187–1192). Elsevier.
- Fossum, T. W. (2019). Small animal surgery (5th ed., pp. 245–267). Elsevier.
- Löwe, G., & Löwe, O. (2021). Notfälle bei Hund und Katze – Ein tierärztlicher Ratgeber. Kynos-Verlag.
- Merck & Co. (2020). Merck veterinary manual (11th ed.). Merck Publishing.
- Nelson, R. W., & Couto, C. G. (2019). Small animal internal medicine (6th ed.). Elsevier.
- Skowronsky, A., & von Reibnitz, C. (2018). Wound care from A–Z. In C. von Reibnitz & A. Skowronsky (Eds.), Wound care from A–Z. Springer.